Note: Your progress in watching these videos WILL NOT be tracked. These training videos are the same videos you will experience when you take the full ProPALS Recertification program. You may begin the training for free at any time to start officially tracking your progress toward your certificate of completion.
Narrow complex tachycardia, also called supraventricular tachycardia or SVT for short, is caused by some sort of stimulus originating above the patient's ventricles, as opposed to the normal stimulus that's generated by the SA node.
In this lesson, we'll take a deeper dive into supraventricular tachycardia for the PALS patient, including looking more closely at an example of what it looks like on an ECG and seeing what findings and measurements lead us to our conclusion.
With SVT, that stimulus comes from a rogue myocardial cell that stimulates an erratic atrial contraction or a series of erratic atrial contractions like those found in patient's with atrial fibrillation and atrial flutter.
Atrial fibrillation (also called AFib or AF) is a quivering or irregular heartbeat (arrhythmia) that can lead to blood clots, stroke, heart failure, and other heart-related complications.
Atrial flutter (AFL) is a common abnormal heart rhythm that starts in the atrial chambers of the heart. When it first occurs, it is usually associated with a fast heart rate.
Pro Tip #1: While these appear to be the same, the difference is in the beat. Atrial flutter and atrial fibrillation are both abnormal heart rhythms. However, in atrial fibrillation, the atria beat irregularly, while in atrial flutter, the atria beat regularly, but faster than usual and more often than the ventricles, so you may have four atrial beats to every one ventricular beat.
The important thing to note with SVT is that it can persist until there is medical intervention, or it can be intermittent and self-limiting, and can come and go without warning.
By looking at an ECG readout alone, SVT can be difficult to differentiate from sinus tachycardia, AFib, or AFL. However, there are things that you can look at to help you determine which rhythm is being displayed.
Now let's take a look at an ECG for a patient in supraventricular tachycardia.
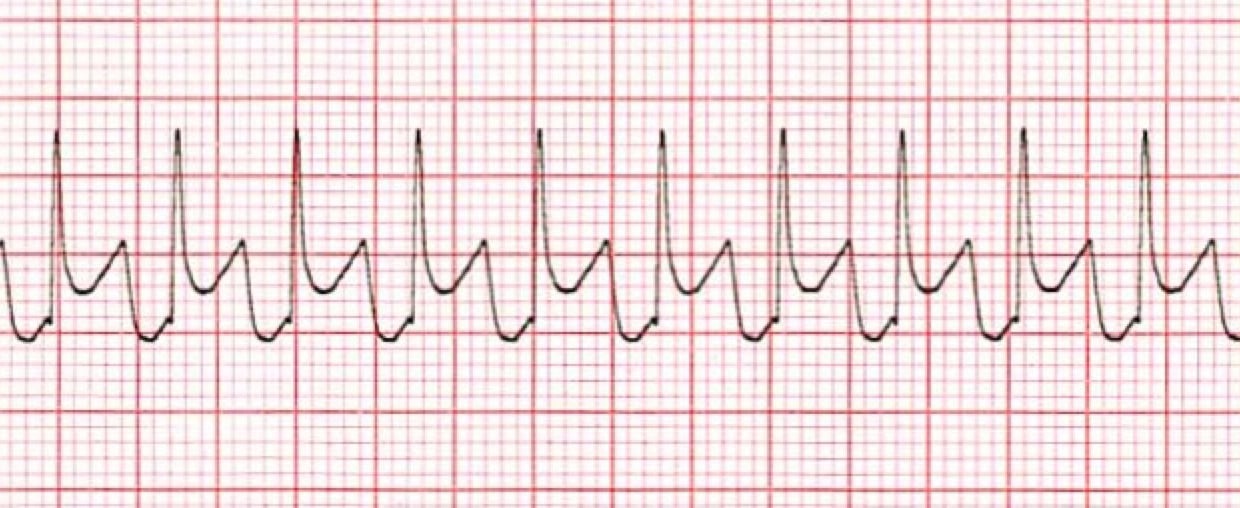
*Supraventricular Tachycardia
1. The Heart Rhythm
The first thing you'll want to look at is the heart rhythm. Does the heart rhythm look regular? Or does it look irregular? In the ECG above, the rhythm is regular.
2. The Heart Rate
Next, you'll want to look at the heart rate of the patient. What is the patient's heart rate? Is it normal? Or is it too slow or too fast? In this case, it's too fast. SVT usually presents with a heart rate of 220 beats per minute in infants or 180 in children.
3. P-Wave
After looking at the heart rate, check to see if the patient's P-waves look normal by asking yourself the following few questions.
- Are the patient's P-waves present? No! P-waves for SVT will either not be present or abnormal, and in this case, they aren't present. And thus, the answers to all other P-wave questions will also be no.
4. PR Interval
Next, look at the PR interval on the patient's ECG readout and ask yourself the following questions:
- Is the PR interval normal, meaning less than .20 seconds or is it contained within one large square on the readout? The answer is no, because there isn't a PR interval.
- Is the PR interval constant? Again, this in non-applicable since there isn't a P-wave.
5. QRS Complex
The last thing you should look at to determine if the sinus rhythm is normal or not is the QRS complex and ask yourself these questions while you do:
- Is the QRS interval less than .09 seconds? Yes, it is.
- Is the QRS complex wide or narrow? In this case, it's narrow.
Pro Tip #2: It's unusual for SVT to present with a wide complex QRS.
- Are the QRS complexes similar in appearance or are there noticeable differences? In this case, we can see that each looks similar.
So, what is your cardiac interpretation? Based on these questions and on the findings from the ECG readout above, it would appear that this patient is in supraventricular tachycardia.
- We have a regular rhythm.
- We have a faster than normal heart rate, and faster than sinus tachycardia, with a rate of 270.
Pro Tip #3: SVT is always more symptomatic than sinus tachycardia. Sinus tachycardia has a rate of 160 – 220 (infants) and 120 – 160 (older children), while SVT has a rate of 220 – 320 (infants) and 160 – 280 (older children).
- The P-waves are missing.
- There is no PR interval.
- The QRS is less than .09 seconds and thus normal.
From the ECG alone, it would indicate that the patient is in SVT. However, patient signs and symptoms must be taken into account to properly identify the rhythm correctly and to determine whether or not treatment is necessary.
Pro Tip #4: Usually a patient with SVT will have a history of vague or non-specific symptoms or palpitations along with sudden onset. In addition, the patient's history is often not compatible with sinus tachycardia. In other words, the patient won't have a fever, won't be dehydrated, and won't be exhibiting any other identifying causes for the SVT.
Unlike with sinus tachycardia, the heart rate doesn't vary with activity, such as when a child is moving around, cries, or becomes agitated.
Keep in mind, though, that if the patient is hemodynamically unstable, such as in hypotension, quick and effective treatment must be provided to correct the abnormal heart rhythm.




